VCS AIR QUALITY
As we approach another fall season here in California, we thought it might be useful to give everyone a refresher on how VCS handles issues of air quality. As we know all too well, fall is fire season here, and smoke drift is a known issue. I wanted to take a moment to share with you how decisions are made regarding air quality.
VCS, like all schools in Sonoma County, follows SCOE’s Air Quality Guidance, which was recently updated. Among those guidelines are the following directions:
- School districts will monitor the air quality index (AQI) using EPA’s AQI monitoring tools at Fire.AirNow.gov, which aggregates data from Purpleair.com and Airnow.gov. This is the site SCOE has confirmed Districts are to use, and we will now use it going forward.
- School activities and closures decisions will be made based on fire.airnow.gov measurements and local conditions, such as the availability and quality of air filtration and direct observation of indoor/outdoor air quality.
- Children with respiratory or heart conditions are vulnerable to poor air quality and may require extra precautions. School districts should advise parents to consult with their child’s health care provider to develop a plan of action before smoke creates a hazardous air situation.
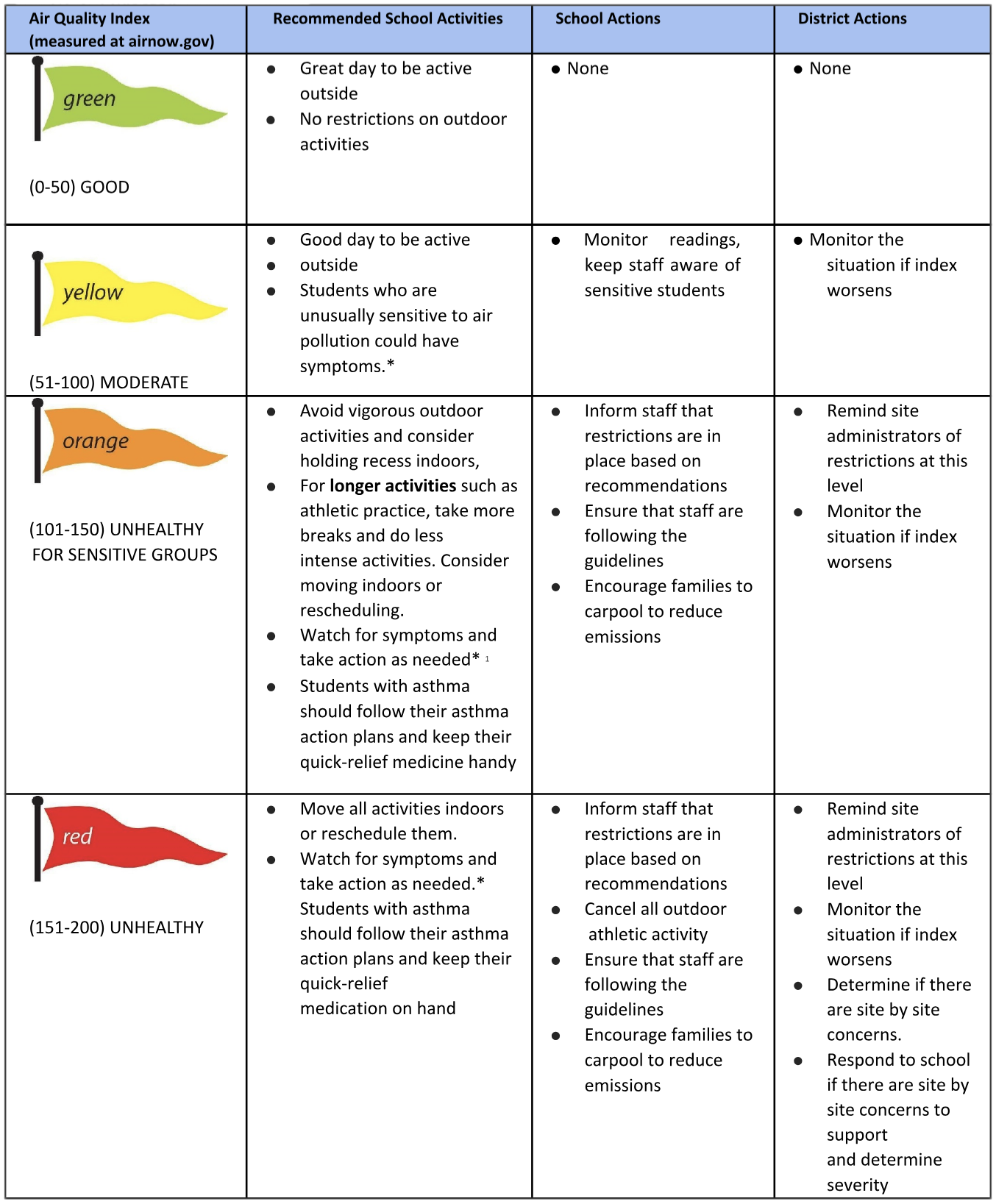
It also includes a chart for what actions school districts should take depending on the air quality (see below).
These are the guidelines we are following. We understand that each family must make their own decisions regarding their students’ health and welfare, and we respect those decisions.
To view SCOE’s complete guidance, please go to:
Sonoma County Schools Air Quality Guidance
Air Quality conditions can change rapidly, so VCS will continue our monitoring, and inform you as needed if things change. If you have any questions, please do not hesitate to reach out to us.
Thank you!
Rebecca Ivanoff
VCS Director
COVID-19
CDPH Public Health Guidance for K-12 Schools, Effective Sept. 30, 2022
All persons with COVID-19 symptoms, regardless of vaccination status or previous infection, should:
• Wear a mask around others for a total of 10 days.
• Self-isolate and test as soon as possible to determine infection status. Knowing one is infected early after symptom onset enables (a) earlier access to treatment options, if indicated (especially for those who may be at risk for severe illness), and (b) notification of exposed persons (close contacts) who may also benefit by knowing if they are infected.
◦ For symptomatic persons who have tested positive within the previous 90 days, using an antigen test is recommended because PCR tests can detect noninfectious viral fragments for up to 90 days.
• If symptoms persist, consider continuing self-isolation and retesting with an antigen or PCR test in 1–2 days if testing negative with an antigen test, particularly if tested during the first 1–2 days of symptoms. Consider repeat testing every 1–2 days for several days if symptoms continue. If any of those tests are positive:
◦ Follow recommended actions below (Table 1).
◦
Contact a healthcare provider about available treatments, especially those at high risk for serious disease or with any questions concerning their care. For more information about available treatments, please see
COVID-19 Treatments (ca.gov).
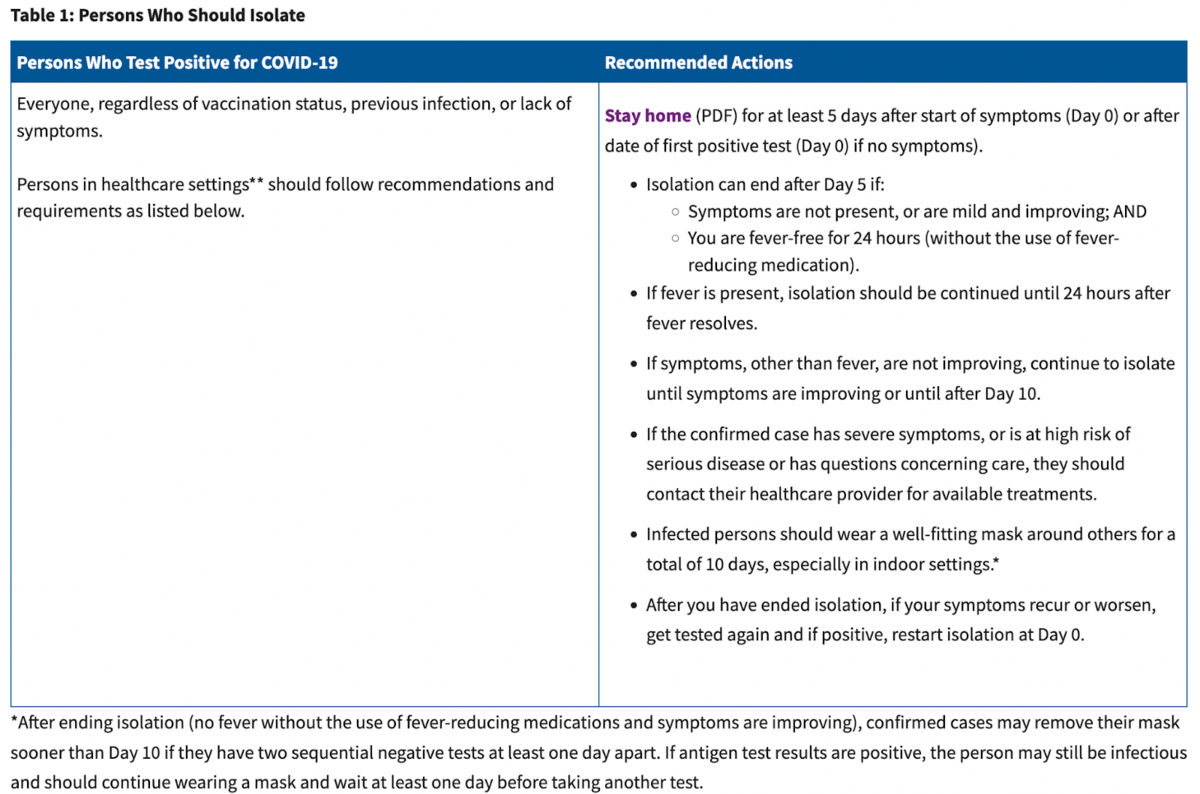
The CDPH updated the following: Individuals infected with COVID-19 may now leave isolation after Day 5 if their symptoms: are not present or are mild and improving, provided they have not had a fever within the past 24 hours and are not taking fever-reducing medication. If the fever is still present after Day 5, isolation should continue until 24 hours after the fever resolves. The CDPH also has ended the recommendation to test in order to leave isolation before Day 10. It is still recommended that infected individuals remain masked for 10 days unless they have two sequential negative tests, one day apart.
